Fort Worth Plastic Surgery
Experience Matters
Trust your transformation to Emily J. Kirby, MD, an award-winning breast and body expert.

Plastic Surgery Expertise
Dr. Kirby’s Awards & Honors













Dr. Emily Kirby has achieved numerous awards and accolades during her career as a Board Certified Plastic Surgeon. She has been recognized as a Castle Connolly Top Doctor since 2019, and is a member of the American Society of Plastic Surgeons and The Aesthetic Society. Dr. Kirby was named a Texas Super Doctor Rising Star from 2016-2017, then a Super Doctor starting in 2018.
She was asked to serve on the Blue Ribbon Panel Review Committee for Super Doctors. Dr. Kirby has been named a Top Doctor by 360 West Magazine and FW Magazine consistently since 2014. In 2018, she was named an Aggie 100 Honoree by Texas A&M University—an honor reserved for the 100 fastest-growing Aggie-owned or Aggie-led businesses in the world.
Plastic Surgery Procedures
Board-certified by the American Board of Plastic Surgery, female plastic surgeon, Dr. Emily J. Kirby, specializes in aesthetic plastic surgery in Fort Worth, Texas.
How do I know the right procedures for me?
Not sure where to start? Come in for your Fort Worth plastic surgery consultation and we’ll listen to your goals and concerns, answer your questions, and help you choose among our large range of surgical and non-surgical rejuvenation procedures. Whether you are looking for breast enhancement with breast implants, brow lift, or premier medical spa services, our highly-experienced aesthetic professionals at Kirby Plastic Surgery would love to meet with you and explain your options.
Dr. Emily J. Kirby
Female Plastic Surgeon Fort Worth
- Board-Certified Plastic Surgeon
- Over 12 years of experience in private practice
- Founder and Medical Director of Kirby Plastic Surgery, Kalos Medical Spa, and City Surgery Center—a Quad A-accredited, state-of-the-art facility located onsite
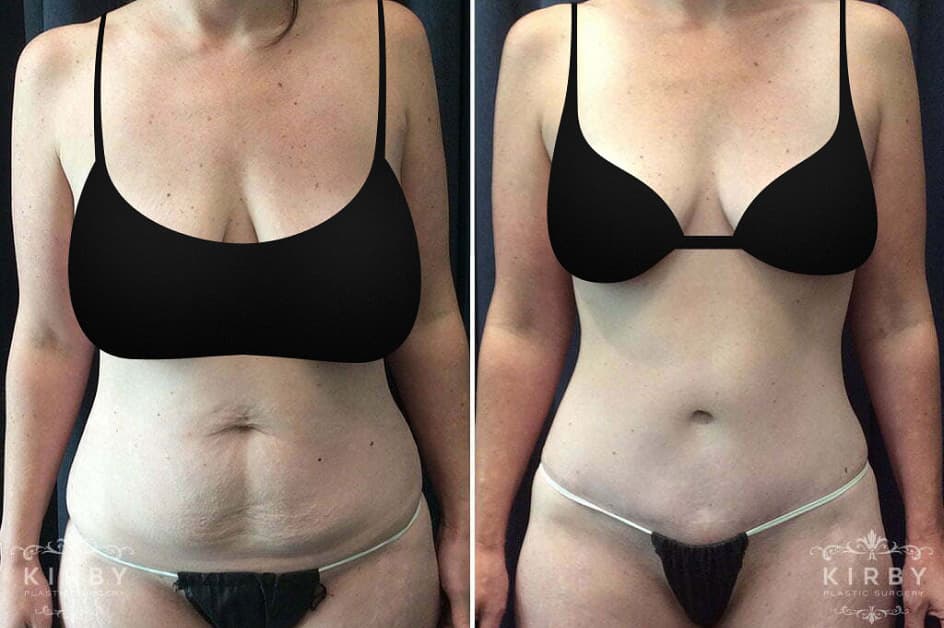
- Specialist in breast surgery and body contouring, including postpartum
- Castle Connolly Top Doctor since 2019
- First female Chief of Plastic Surgery, Texas Health Resources Harris Methodist Hospital


Patient Reviews
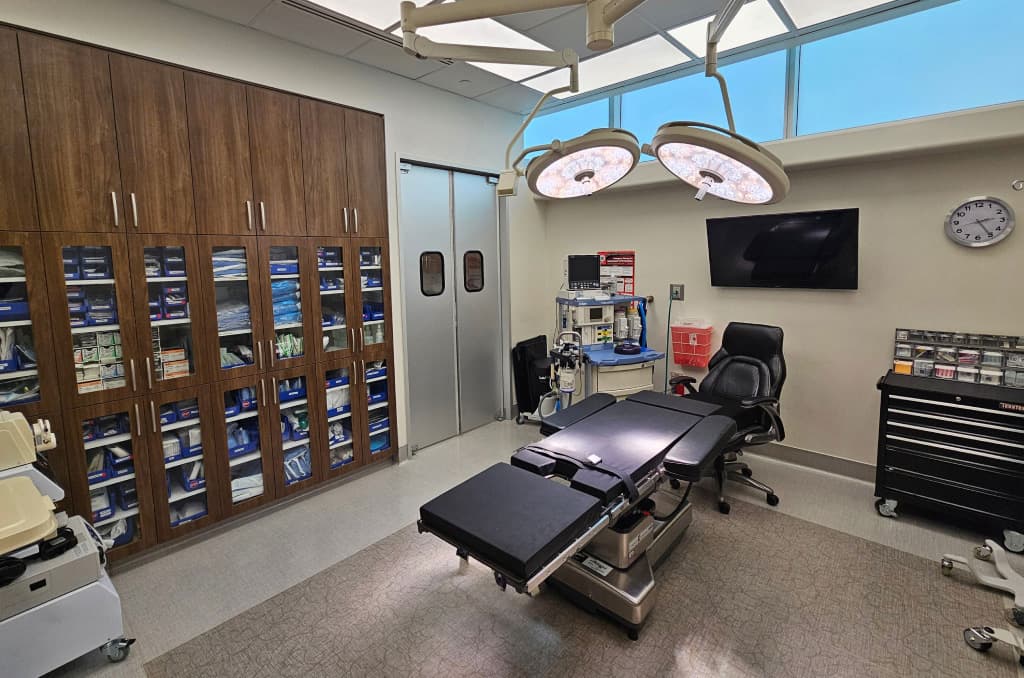
City Surgery Center
Our on-site, accredited surgical suite
Instead of heading to a hospital or other public surgical facility for your procedure, you can enjoy the privacy and luxury of our on-site operating room, designed to facilitate safe, top-quality care in a spa-like setting.
Serving the greater Fort Worth, Texas area
It’s an honor to serve greater Fort Worth and you are our top priority each time you come through the door! We are located in the Shops at Clearfork, just a few minutes from downtown Fort Worth. We are convenient to many area neighborhoods, including Ridglea Hills, the Cultural District, Stockyards, River Oaks, Westover Hills, Tanglewood, and TCU. It’s especially easy to reach us if you are in the 76107, 76109, 76110, 76008 or 76126 zip codes. Visit our Fort Worth office directions page for more about our business hours or driving directions.